The pandemic has irreversibly changed America’s health care system. Here’s why we will all be feeling the consequences of delayed care for years to come
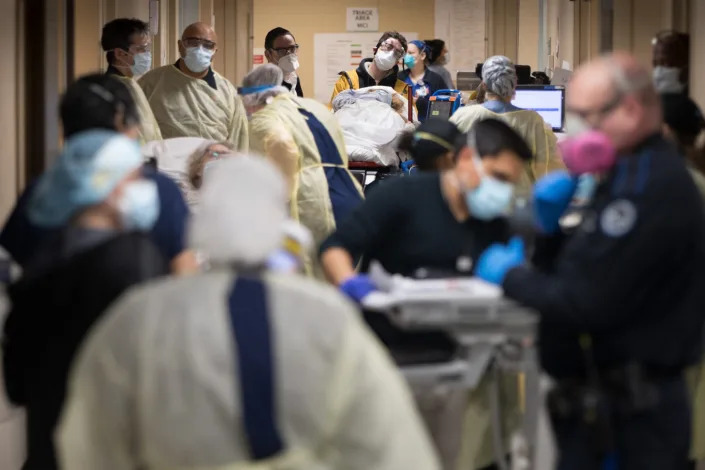
Elazer R. Edelman, Mike Mussallem
Tue, February 21, 2023
The consequences of the latest wave of flu and RSV (respiratory syncytial virus) cases coupled with the ongoing spread of COVID-19 variants are starting to play out for those with long-standing medical conditions who are waiting even longer for nonemergency procedures and doctors’ visits or deferring care altogether to avoid overcrowded facilities.
This is not just an issue in the United States. In the U.K., more than 7 million people are currently on elective surgery waitlists after years of pandemic-related disruptions.
It’s an all-too-familiar tale for those of us in health care who witnessed firsthand the devastating toll of postponed checkups and procedures as hospitals conserved resources for the pressing pandemic response. A procedure’s urgency was often left to interpretation—and indefinite cancellations proved catastrophic for many.
The backlog of deferred treatment and resulting long-term health consequences, including a significant decline in overall life expectancy, will continue to impact public health for years, if not decades, much like the 1918 Spanish flu epidemic, which attacked a fifth of the world's population and continued to affect public health for years.
Now is the time to thoughtfully and strategically reevaluate our policy approach to nonemergent medical care and surgical procedures amid health crises. We know that there are consequences to making profound policy decisions—especially in health care—and therefore we must learn and directly confront them, to better serve the ongoing needs of our patients.
The downstream effects of deprioritizing “elective” care
It is important to understand that elective is not the same as optional. More than 90% of surgeries are considered elective, which means these are nonemergency procedures that can be scheduled in advance. Though sometimes labeled “nonessential,” these measures that range from organ transplants to cancer operations are often vital to people’s health and well-being.
We didn’t need the pandemic to tell us that delaying care can lead to dire consequences for patients. Elective surgery delays can be detrimental in both preventive and curative care, allowing disease progression or leading to premature death. In 2020, Mayo Clinic warned that halting colon cancer procedures for more than four months would result in over 30,000 fatalities, while a study from The BMJ found that an eight-week delay in breast cancer treatment increased the risk of death by 17%. After a 12-week delay, mortality rates jumped to 26%.
Research on treatment disruption for patients with aortic stenosis, a narrowing of the heart valve opening that can be deadly if not treated quickly, also showed dire outcomes. One study published in JAMA found that nearly three months after elective procedures were halted amid COVID, more than 30% of aortic stenosis patients who deferred care required emergency transcatheter aortic valve replacement (TAVR) or died.
A compounding workforce crisis
As demand for medical care amid the pandemic increased exponentially, supply simply could not keep up. Hospitals were triaging extreme patient volumes while navigating unprecedented staffing and resource shortages, adding to the cyclical set of issues straining a less-than-robust system.
A lack of funding and resources, along with rising anxiety, depression, and burnout, contributed to a mass exodus of frontline workers. More than half-a-million health care and social service employees left the industry each month in 2022 and more than a third of nurses say they’re planning to quit soon. The American Hospital Association penned a letter to the U.S. House of Representatives Energy and Commerce Committee and declared the shortages “a national emergency.” Staffing needs are as urgent as ever, with 16 million working-age Americans still struggling with long COVID-19, resulting in around $170 billion in lost wages annually. These staggering shortages and rising backlogs continue to limit the number of nonemergent procedures that can be performed.
Rethinking pandemic preparedness
Pandemics are disruptive, not only because of their direct assault on individual health but also due to the ripple effects of the policy decisions they necessitate. As we navigate the aftermath and substantial costs of COVID-19 along with this new onslaught of respiratory illnesses, it is more important than ever to reflect on the unintended consequences of restrictions imposed on health care operations. These include recalibrating to clear backlogs as quickly as possible and ensuring access to crucial, often lifesaving procedures.
As part of the health care ecosystem, we have a responsibility to patients, medical workers, and ourselves to rethink how we prioritize resources and evaluate the holistic impacts of policy on public health in response to a crisis.
Innovation is driven by evidence and the same should be true for our health care policies. It is incumbent upon us to identify timely real-world evidence to elucidate the effects of policy changes so they can be adaptive and agile enough to provide access to critical interventions and procedures. Only then can we ensure continuous care for all patients throughout the next wave—and pandemics yet to come.
Elazer R. Edelman, M.D., Ph.D., is professor of medicine at Harvard Medical School and professor of medical engineering and science at MIT. Mike Mussallem is the chairman and CEO of Edwards Lifesciences.
The opinions expressed in Fortune.com commentary pieces are solely the views of their authors and do not necessarily reflect the opinions and beliefs of Fortune.
The opinions expressed in Fortune.com commentary pieces are solely the views of their authors and do not necessarily reflect the opinions and beliefs of Fortune.

No comments:
Post a Comment