Pharmacy benefit managers (PBMs) under the microscope for their role in high drug prices have often cited their reportedly slim profit margins as evidence that they do not drive up costs. The three leading PBMs, which control about 80% of the prescription drug market, have historically reported profit margins of 4% to 7%, among the lowest in the healthcare industry.
A new white paper from the USC Schaeffer Center for Health Policy & Economics demonstrates that these slim margins are dramatically influenced by the accounting practices PBMs elect to employ. The paper also shows how efforts to assess PBM profits have become more challenging after these companies merged with healthcare conglomerates that own other players in the pharmaceutical supply chain.
States in recent years have advanced or considered numerous measures seeking to increase PBM transparency, and Congress is currently pursuing legislation to reform PBM practices. The Federal Trade Commission, meanwhile, continues to scrutinize PBMs after accusing leading firms of inflating drug costs through strategies like rebates, markups and preferential treatment of affiliated pharmacies.
“Accounting practices make it difficult to judge the health and efficiency of the PBM market, particularly as dominant firms have become part of larger, more complex companies,” said lead author Karen Mulligan, a research scientist at the Schaeffer Center. “Greater financial disclosure requirements for PBMs are needed to develop a better picture of how PBMs make money and the extent to which these practices may raise costs for consumers.”
How accounting choices drive margins
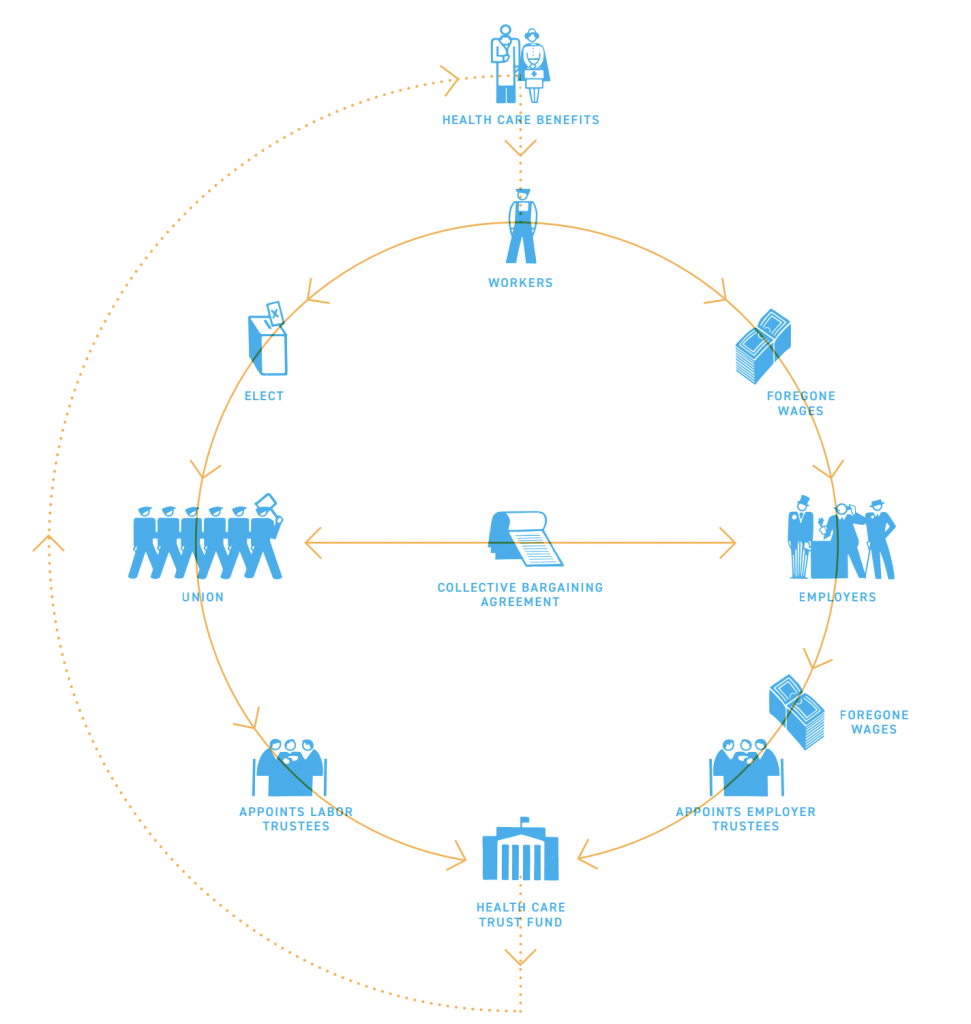
PBMs sit at the center of the pharmaceutical supply chain, acting as intermediaries that pay pharmacies and negotiate rebates with drug manufacturers on behalf of insurers. PBMs retain transaction fees and a portion of manufacturer rebates while passing along payments between manufacturers, insurers and pharmacies.
Historically, PBMs have included these “pass-through payments” in financial reporting. This may also include the share of rebates sent directly to the insurer. While allowed under professional accounting guidelines, this practice may add hundreds of billions of dollars to PBMs’ reported revenue or expenses without affecting their actual earnings. This obscures key determinants of PBMs’ profitability, including the role of rebates, fees and other payments.
Using a simplified example with typical transaction fees and rebates, the white paper illustrates how accounting choices can produce vastly different profit margins for a hypothetical drug listed at $360. If pass-through payments were reported as revenues or expenses, the PBM’s margin would be 10% – or slightly higher at 13% if manufacturer rebates passed to the insurer were not reported. However, the margin jumps to 87% if pass-through payments were not reported at all. (See Figure 5 in the white paper.)
Vertical integration in the healthcare industry has further blurred PBMs’ financial picture. In the past decade, the three dominant PBMs have become part of diverse healthcare corporations that also own insurers, specialty pharmacies and group purchasing organizations (GOPs) that negotiate discounts.
Under this structure, payments between the PBM, insurer and the specialty pharmacy become internal transfers invisible to the public. Using the same hypothetical $360 drug as the previous example, the white paper shows how the publicly reported profit margin can be half of what’s recorded internally, as dollars are shifted to other units within the PBM’s parent company. (See Figure 6.)
Transparency reforms should illuminate revenue streams
The researchers suggest that policymakers consider requiring PBMs to exclude pass-through payments from financial reporting, as regulators have done for intermediaries in other industries.
Policymakers should also consider reforming financial reporting requirements so that healthcare conglomerates provide separate reporting for each distinct business unit, rather than allowing PBM operations to be combined with other units like specialty pharmacy. Further, requiring disclosure of internal transfers and pass-through payments in these companies would provide clarity about what’s driving profits.
“True transparency requires greater visibility into profit flows hidden inside increasingly complex corporate structures,” said co-author Darius Lakdawalla, chief scientific officer at the Schaeffer Center and the Quintiles Chair of Pharmaceutical Development and Regulatory Innovation at the USC Mann School. “Building a more efficient and sustainable pharmaceutical supply chain starts with a better understanding of where dollars are flowing.”
Article Publication Date
22-Jan-2026
COI Statement
This white paper was supported by the Schaeffer Center. A complete list of supporters of the Schaeffer Center can be found in our annual report online.
For more than a decade, hospitals have worked to help older adults avoid repeated inpatient stays, incentivized by a federal program that cuts Medicare reimbursements if hospitals have higher-than-expected rates of readmissions for people with certain conditions.
The Hospital Readmissions Reduction Program has helped spur innovation, including initiatives to better prepare patients and their families to manage care after hospitalization, and to support them virtually at home.
But a new University of Michigan study finds that these financial penalties have hit some hospitals harder than they should, even if those hospitals have done a reasonable job at keeping people with heart failure, pneumonia and other serious conditions from ending up back in a hospital within a month of leaving one.
Such hospitals have been paying inflated readmission penalties for a seemingly unrelated reason: They happen to serve higher percentages of older adults who have chosen to enroll in Medicare Advantage plans run by private insurance companies.
So what’s the connection?
Currently, the federal government only grades hospitals on their readmission performance for older adults with traditional Medicare, which is run by the federal government. Data from Medicare Advantage are not currently included in the calculations that determine these penalties.
This is a problem, because Medicare Advantage enrollees tend to be healthier than traditional Medicare beneficiaries. But the readmission penalty program’s risk-adjustment is unable to capture these differences.
So, the researchers find, hospital performance looks worse for hospitals treating fewer traditional Medicare beneficiaries and more Medicare Advantage enrollees, even if those hospitals take the same actions to prevent readmissions as other hospitals.
The study, published in JAMA Network Open, suggests that not incorporating Medicare Advantage data results in an unwarranted redistribution of nearly $300 million a year in readmission penalties across hospitals nationwide. That’s more than half the total amount of readmissions penalties incurred each year across all hospitals.
Penalties are publicly reported every year and covered by the news media.
The Centers for Medicare and Medicaid Services has issued a rule to begin using Medicare Advantage data in the program. But even when it takes effect later this year, it will not affect hospital penalties for several years.
An unintended consequence with major consequences
The analysis shows an unintended consequence of the intersection between two major health policies of the last 15 years: the rapid rise in Medicare plan enrollment, and the HRRP, says senior author Geoffrey Hoffman, Ph.D., a professor at the U-M School of Nursing and member of the U-M Institute for Healthcare Policy and Innovation.
“Medicare Advantage has experienced extraordinary growth in the past decade, yet policymakers haven’t caught up with implications of this growth for Medicare payment policy that is based purely on traditional Medicare enrollment,” says Hoffman. “The omission of Medicare Advantage data highlights the continuing issue of inadequate measurement of patient risk in the Hospital Readmission Reduction Program, with important implications for the penalties that hospitals face.”
When the HRRP started calculating readmission rates in 2012, only 29% of older adults and people with disabilities chose Medicare Advantage plans.
Today, it’s 54%. But the distribution is not even across the country.
Hoffman and lead author Zoey Chopra, M.A., mapped that distribution and divided more than 3,200 hospitals into five groups based on the MA enrollment levels in 1,486 counties.
Chopra is working toward both a medical degree in the U-M Medical School and a Ph.D. in economics in the U-M College of Literature, Science and the Arts. He is a Medical Scientist Training Program fellow at the Medical School.
Differences in hospitals and populations
The hospitals in the areas with the highest Medicare Advantage enrollment were much more likely to be larger, nonprofit, teaching-oriented and in urban areas than hospitals in the areas with the lowest levels of Medicare Advantage enrollment.
Even when the researchers took into account an aspect of the readmission penalty program that only judges hospitals against groups of their peer hospitals, they still found that the Medicare Advantage enrollment rate mattered.
Past studies have shown that older adults who choose Medicare Advantage plans tend to be in the younger age range of eligibility, and to have fewer serious health conditions.
Hoffman has studied patterns of migration back to traditional Medicare by adults who had previously chosen Medicare Advantage plans, and factors that cause older adults to leave a Medicare Advantage plan for another Medicare Advantage plan or traditional Medicare.
Even though the readmission penalty program adjusts penalties based on the health risks of hospitals’ patients with the conditions that are included in the program, the lack of Medicare Advantage data could be a source of bias, he said.
Areas with more Medicare Advantage enrollees may end up with higher-risk traditional Medicare beneficiaries, because healthier enrollees migrate to Medicare Advantage. But those risk differences can’t be captured in the data models used by CMS. Therefore, by basing the program’s penalties only on traditional Medicare enrollees, hospitals with more Medicare Advantage patients are at greater, unwarranted risk of readmission penalties.
“Our study observes an inadvertent consequence of restricting the readmissions program to traditional Medicare participants,” said Chopra. “At the time of the HRRP’s rollout, this made sense, given lower enrollment and concerns about accuracy of the Medicare Advantage data. However, including Medicare Advantage data now appears imperative to avoid unnecessary penalties for hospitals treating relatively more private pay patients.”
Potential solutions
The new policy taking effect later this year rule will add Medicare Advantage data to HRRP calculations of readmissions, but Hoffman and Chopra have concerns about the completeness of what may be available. Risk-coding and policy differences across Medicare Advantage and traditional Medicare could also complicate comparisons of hospital performance.
It will also base penalties on the last two years’ worth of readmission data, instead of three. While the inclusion of Medicare Advantage data nearly doubles the amount of data used for comparisons, given concerns about data completeness and accuracy, this change may nonetheless make it harder statistically to see how hospitals have really done on keeping readmissions as low as possible, Hoffman said.
In addition to the rule, they suggest, CMS could consider factoring the percentage of Medicare Advantage enrollees in a hospital’s area or patient base into the calculations for its readmission rate and potential penalty.
The study was funded by the National Institute on Aging of the National Institutes of Health (RO1AG074944, T32AG000221). Chopra’s funding is through the Population Studies Center at the U-M Institute for Social Research. Andrew Ryan, Ph.D., of Brown University is a co-author of the study.
Hospital Readmission Reduction Program Penalties for Hospitals with High Medicare Advantage Penetration, JAMA Network Open, DOI:10.1001/jamanetworkopen.2025.54972
Method of Research
Data/statistical analysis
Subject of Research
People
Article Title
Hospital Readmission Reduction Program Penalties for Hospitals with High Medicare Advantage Penetration
Article Publication Date
22-Jan-2026