AMERIKAN EXCEPTIONALISM;
Parents Are Being Asked to Pay the Cost of Delivering Their Babies in AdvanceFOR PROFIT HEALTHCARE
Childbirth is already unaffordable for many. Now some are being asked to pay the bill before they even go into labor.By Renuka Rayasam ,
December 1, 2024
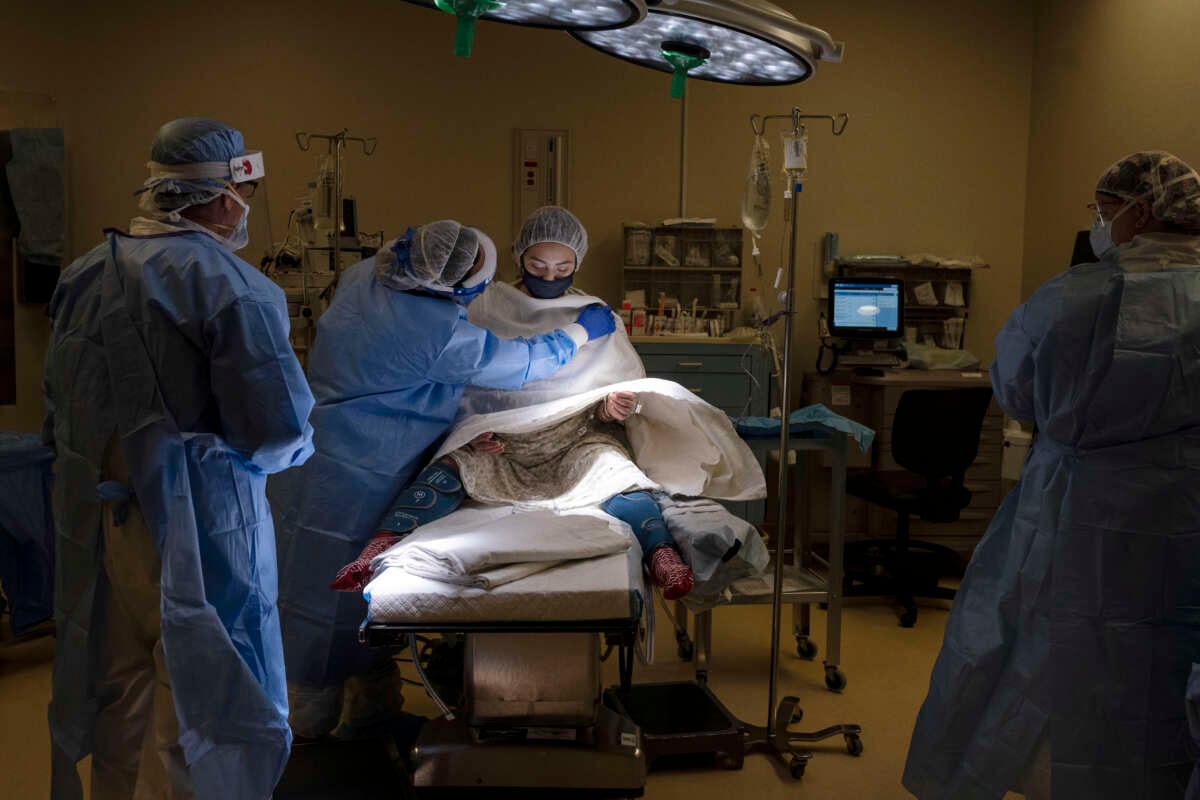
A young mother is supported by nurses as she is prepped by the anesthesiologist for an epidural before a cesarian section to deliver twins at the Women's Hospital at the the Doctors Hospital at Renaissance in McAllen, Texas, on July 7, 2020.
Lynsey Addario / Getty Images
In April, just 12 weeks into her pregnancy, Kathleen Clark was standing at the receptionist window of her OB-GYN’s office when she was asked to pay $960, the total the office estimated she would owe after she delivered.
Clark, 39, was shocked that she was asked to pay that amount during this second prenatal visit. Normally, patients receive the bill after insurance has paid its part, and for pregnant women that’s usually only when the pregnancy ends. It would be months before the office filed the claim with her health insurer.
Clark said she felt stuck. The Cleveland, Tennessee, obstetrics practice was affiliated with a birthing center where she wanted to deliver. Plus, she and her husband had been wanting to have a baby for a long time. And Clark was emotional, because just weeks earlier her mother had died.
“You’re standing there at the window, and there’s people all around, and you’re trying to be really nice,” recalled Clark, through tears. “So, I paid it.”
On online baby message boards and other social media forums, pregnant women say they are being asked by their providers to pay out-of-pocket fees earlier than expected. The practice is legal, but patient advocacy groups call it unethical. Medical providers argue that asking for payment up front ensures they get compensated for their services.
Related Story
In April, just 12 weeks into her pregnancy, Kathleen Clark was standing at the receptionist window of her OB-GYN’s office when she was asked to pay $960, the total the office estimated she would owe after she delivered.
Clark, 39, was shocked that she was asked to pay that amount during this second prenatal visit. Normally, patients receive the bill after insurance has paid its part, and for pregnant women that’s usually only when the pregnancy ends. It would be months before the office filed the claim with her health insurer.
Clark said she felt stuck. The Cleveland, Tennessee, obstetrics practice was affiliated with a birthing center where she wanted to deliver. Plus, she and her husband had been wanting to have a baby for a long time. And Clark was emotional, because just weeks earlier her mother had died.
“You’re standing there at the window, and there’s people all around, and you’re trying to be really nice,” recalled Clark, through tears. “So, I paid it.”
On online baby message boards and other social media forums, pregnant women say they are being asked by their providers to pay out-of-pocket fees earlier than expected. The practice is legal, but patient advocacy groups call it unethical. Medical providers argue that asking for payment up front ensures they get compensated for their services.
Related Story

Georgia Maternal Mortality Board Dissolved Over Report on Abortion Ban Deaths
One critic described the move as an “attempt to conceal the deadly consequences” of Georgia’s abortion ban.
By Chris Walker , TruthoutNovember 25, 2024
How frequently this happens is hard to track because it is considered a private transaction between the provider and the patient. Therefore, the payments are not recorded in insurance claims data and are not studied by researchers.
Patients, medical billing experts, and patient advocates say the billing practice causes unexpected anxiety at a time of already heightened stress and financial pressure. Estimates can sometimes be higher than what a patient might ultimately owe and force people to fight for refunds if they miscarry or the amount paid was higher than the final bill.
Up-front payments also create hurdles for women who may want to switch providers if they are unhappy with their care. In some cases, they may cause women to forgo prenatal care altogether, especially in places where few other maternity care options exist.
It’s “holding their treatment hostage,” said Caitlin Donovan, a senior director at the Patient Advocate Foundation.
Medical billing and women’s health experts believe OB-GYN offices adopted the practice to manage the high cost of maternity care and the way it is billed for in the U.S.
When a pregnancy ends, OB-GYNs typically file a single insurance claim for routine prenatal care, labor, delivery, and, often, postpartum care. That practice of bundling all maternity care into one billing code began three decades ago, said Lisa Satterfield, senior director of health and payment policy at the American College of Obstetricians and Gynecologists. But such bundled billing has become outdated, she said.
Previously, pregnant patients had been subject to copayments for each prenatal visit, which might lead them to skip crucial appointments to save money. But the Affordable Care Act now requires all commercial insurers to fully cover certain prenatal services. Plus, it’s become more common for pregnant women to switch providers, or have different providers handle prenatal care, labor, and delivery — especially in rural areas where patient transfers are common.
Some providers say prepayments allow them to spread out one-time payments over the course of the pregnancy to ensure that they are compensated for the care they do provide, even if they don’t ultimately deliver the baby.
“You have people who, unfortunately, are not getting paid for the work that they do,” said Pamela Boatner, who works as a midwife in a Georgia hospital.
While she believes women should receive pregnancy care regardless of their ability to pay, she also understands that some providers want to make sure their bill isn’t ignored after the baby is delivered. New parents might be overloaded with hospital bills and the costs of caring for a new child, and they may lack income if a parent isn’t working, Boatner said.
In the U.S., having a baby can be expensive. People who obtain health insurance through large employers pay an average of nearly $3,000 out-of-pocket for pregnancy, childbirth, and postpartum care, according to the Peterson-KFF Health System Tracker. In addition, many people are opting for high-deductible health insurance plans, leaving them to shoulder a larger share of the costs. Of the 100 million U.S. people with health care debt, 12% attribute at least some of it to maternity care, according to a 2022 KFF poll.
Families need time to save money for the high costs of pregnancy, childbirth, and child care, especially if they lack paid maternity leave, said Joy Burkhard, CEO of the Policy Center for Maternal Mental Health, a Los Angeles-based policy think tank. Asking them to prepay “is another gut punch,” she said. “What if you don’t have the money? Do you put it on credit cards and hope your credit card goes through?”
Calculating the final costs of childbirth depends on multiple factors, such as the timing of the pregnancy, plan benefits, and health complications, said Erin Duffy, a health policy researcher at the University of Southern California’s Schaeffer Center for Health Policy and Economics. The final bill for the patient is unclear until a health plan decides how much of the claim it will cover, she said.
But sometimes the option to wait for the insurer is taken away.
During Jamie Daw’s first pregnancy in 2020, her OB-GYN accepted her refusal to pay in advance because Daw wanted to see the final bill. But in 2023, during her second pregnancy, a private midwifery practice in New York told her that since she had a high-deductible plan, it was mandatory to pay $2,000 spread out with monthly payments.
Daw, a health policy researcher at Columbia University, delivered in September 2023 and got a refund check that November for $640 to cover the difference between the estimate and the final bill.
“I study health insurance,” she said. “But, as most of us know, it’s so complicated when you’re really living it.”
While the Affordable Care Act requires insurers to cover some prenatal services, it doesn’t prohibit providers from sending their final bill to patients early. It would be a challenge politically and practically for state and federal governments to attempt to regulate the timing of the payment request, said Sabrina Corlette, a co-director of the Center on Health Insurance Reforms at Georgetown University. Medical lobbying groups are powerful and contracts between insurers and medical providers are proprietary.
Because of the legal gray area, Lacy Marshall, an insurance broker at Rapha Health and Life in Texas, advises clients to ask their insurer if they can refuse to prepay their deductible. Some insurance plans prohibit providers in their network from requiring payment up front.
If the insurer says they can refuse to pay up front, Marshall said, she tells clients to get established with a practice before declining to pay, so that the provider can’t refuse treatment.
Clark said she met her insurance deductible after paying for genetic testing, extra ultrasounds, and other services out of her health care flexible spending account. Then she called her OB-GYN’s office and asked for a refund.
“I got my spine back,” said Clark, who had previously worked at a health insurer and a medical office. She got an initial check for about half the $960 she originally paid.
In August, Clark was sent to the hospital after her blood pressure spiked. A high-risk pregnancy specialist — not her original OB-GYN practice — delivered her son, Peter, prematurely via emergency cesarean section at 30 weeks.
It was only after she resolved most of the bills from the delivery that she received the rest of her refund from the other OB-GYN practice.
This final check came in October, just days after Clark brought Peter home from the hospital, and after multiple calls to the office. She said it all added stress to an already stressful period.
“Why am I having to pay the price as a patient?” she said. “I’m just trying to have a baby.”
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF — an independent source of health policy research, polling, and journalism. Learn more about KFF
Renuka Rayasam is a senior correspondent at Kaiser Health News.

No comments:
Post a Comment